The relationship between artificial intelligence and electronic health records has shifted dramatically over the past year. What was once a promising pilot initiative is now standard infrastructure: 71% of U.S. hospitals were running at least one EHR-integrated predictive AI tool by the end of 2024, up from 66% just a year earlier. And that number keeps climbing. For healthcare organizations still weighing whether and how to move forward, the question is no longer if AI belongs in EHR systems, it's how to integrate it well.
This guide covers the core benefits, persistent challenges, and the most important recent developments in AI-EHR integration, including what the latest research says about burnout, documentation time savings, and where the technology is heading next.
Key Takeaways
AI-EHR adoption has reached the majority of U.S. hospitals: 71% of U.S. hospitals now use at least one EHR-integrated predictive AI tool, with adoption accelerating sharply year over year.
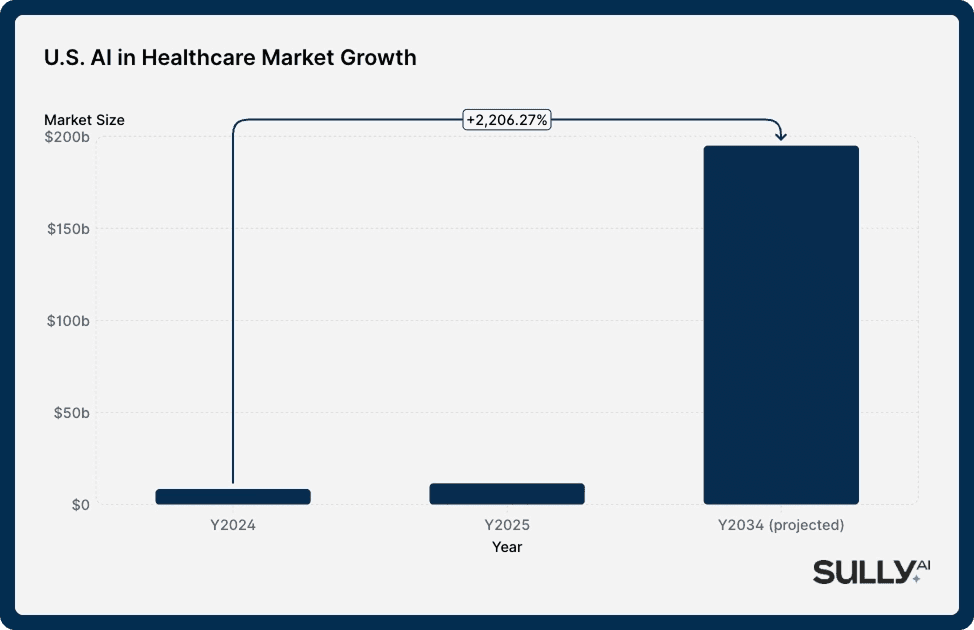
The market is growing at an extraordinary pace: The U.S. AI in healthcare market reached $11.57 billion in 2025 and is projected to exceed $194 billion by 2034; a 37% compound annual growth rate.
AI scribes are the breakout clinical application: Ambient scribing generated $600 million in 2025, 2.4x year-over-year growth, and a Yale School of Medicine study found physician burnout dropped from 51.9% to 38.8% after just one month of use.
Documentation burden remains healthcare's core pain point: Physicians historically spend twice as much time on documentation as with patients, and AI tools cutting that burden are now the single most-funded category in healthcare AI.
EHR vendors are bringing AI in-house: Epic, Oracle Health, and athenahealth have all launched native AI features, meaning AI-EHR integration is increasingly built in, not bolted on.
Why AI Integration with EHR Systems Matters More Than Ever
Electronic health records were transformative when they arrived. They replaced paper charts, enabled data sharing across care teams, and made patient history accessible at the point of care. But they also created an unintended crisis.
Physicians now spend more time in the EHR than with their patients. According to the American Medical Association, documentation time "steals time" from patient care, extending work into evenings and weekends in what clinicians call "pajama time." The AMA notes that 43.2% of physicians reported at least one burnout symptom in 2024, an improvement from 53% in 2022, but still alarmingly high.
This is where AI steps in. Not to replace the EHR, but to make it work the way it was always supposed to: quietly in the background, reducing friction so clinicians can focus on care.
"The time that I spend documenting steals time that I have to be with my patients, which is what brings me joy." - AMA President Jesse Ehrenfeld, MD, MPH
The scale of the opportunity is enormous. Medical documentation and back-office revenue cycle management together account for 60% of healthcare IT spend, creating a $38 billion addressable market for AI to improve established workflows. That's not speculative upside, it's where healthcare money is already flowing.
The Numbers Behind AI-EHR Adoption
By 2025/2026, the picture became much clearer:
66% of U.S. physicians are now using health AI tools, up from 38% in 2023, a 78% increase in a single year
Healthcare organizations are deploying commercial AI at 2.2x the rate of the broader U.S. economy
22% of providers are using domain-specific AI tools, up from just 3% two years prior
$1.4 billion in healthcare AI spending was recorded in 2025, nearly triple the prior year
The bottom line is that AI-EHR integration is no longer a frontier technology. For most organizations, it's becoming standard practice.
The Core Benefits of Integrating AI with EHR Systems
Dramatically Reduced Documentation Burden
The single most powerful benefit of AI in EHR systems right now is the reduction in documentation time. Ambient AI scribes (tools that listen to patient-provider conversations and auto-generate clinical notes) are delivering results that weren't achievable just two years ago.
Research from Duke University found that AI documentation tools cut note-taking time by approximately 20% and reduced after-hours documentation by about 30%. A study published in JAMA Network Open from the University of Chicago found that clinicians using ambient scribes spent 8.5% less total time in the EHR, with a more than 15% drop specifically in time spent composing notes. Some implementations go further: AAMC-reported data on ambient tools shows physicians seeing five more patients per day while spending up to 50% less time on documentation per visit.
These aren't marginal efficiency gains. They're practice-changing.
Less pajama time: Clinicians complete notes during or immediately after visits, rather than after hours
Fewer transcription errors: AI captures and structures information directly from conversation, reducing copy-paste errors common in manual EHR entry
Better note quality: Natural language processing (NLP) identifies clinically relevant information, often producing more complete notes than manual documentation
Faster billing cycles: Documentation completion at point-of-care accelerates coding and claims processing
Meaningful Reduction in Physician Burnout
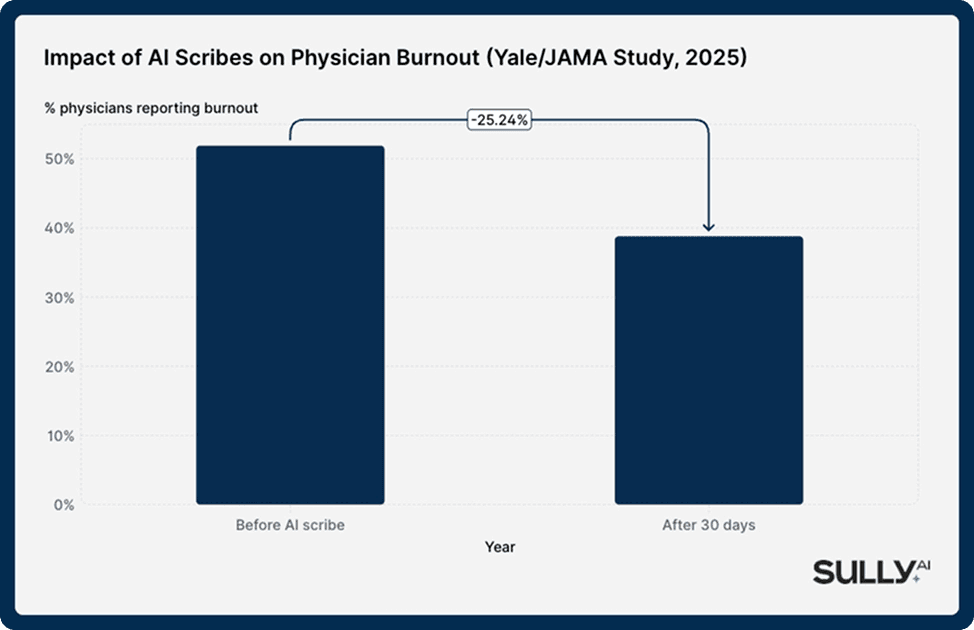
Perhaps the most consequential finding from recent research is what AI scribes do to burnout, not just productivity. In a landmark multicenter study published in JAMA Network Open and highlighted by Yale School of Medicine, 263 physicians across six U.S. health systems were surveyed before and 30 days after adopting an AI scribe. The results were striking: the percentage of physicians reporting burnout fell from 51.9% to 38.8%, ****representing 74% lower odds of experiencing burnout.
This matters beyond individual wellbeing. When a physician leaves practice, it costs health systems between $800,000 and $1.3 million in recruitment and lost productivity. AI scribes, in that context, aren't just a quality-of-life improvement, they're a material financial and operational intervention.
Improved Patient Care Through Predictive Analytics
When AI is integrated into EHR data streams, it can do something no clinician has time to do manually: continuously scan patient records for emerging risk patterns and generate early warnings before conditions worsen.
Key clinical applications include:
Early disease detection: AI models analyze biometric trends, lab values, and historical patterns to flag early signs of chronic conditions like diabetes or cardiovascular disease before they become clinically apparent
Risk stratification: By combining medical history, lifestyle factors, and real-time vitals, AI tools identify high-risk patients who need proactive intervention, not just reactive care
Sepsis prediction: Hospitals are using EHR-integrated AI models to predict sepsis risk hours before it would otherwise be identified, enabling earlier treatment and better outcomes
Readmission prevention: Predictive models flag patients at high risk of 30-day readmission, allowing care teams to intervene with targeted follow-up
"AI algorithms integrate and analyze diverse data sources, EHRs, real-time vital signs, medical history, environmental factors, to understand patient context dynamically." - Grand View Research, 2025
Automated Clinical Workflows and Administrative Efficiency
Beyond documentation, AI is automating the administrative layer that surrounds clinical work. Tasks that once consumed clinical staff hours are increasingly handled by AI agents embedded in or connected to the EHR:
Prior authorization: AI is transforming what was described by Menlo Ventures as "healthcare's most reviled administrative process." The prior auth AI market reached $100+ million in 2025, growing 10x year over year, with systems extracting data from EHRs, applying clinical reasoning, and submitting requests automatically
Appointment scheduling: AI agents manage scheduling, rescheduling, and patient routing with minimal staff involvement
Insurance verification and claims: Tasks that once took hours can be completed in minutes with RPA and AI integration
Medical coding: AI coding tools analyze clinical notes and suggest accurate ICD and CPT codes, reducing denials and improving revenue cycle performance
Deloitte's 2025 Global Healthcare Executive Outlook found that 60% of healthcare executives globally are prioritizing investment in core technologies including EHR and enterprise resource planning, signaling that modernization is now a strategic imperative, not a nice-to-have.
Smarter, More Interoperable Data Sharing
One of AI's underappreciated benefits in EHR integration is what it does for interoperability. Healthcare data has historically been siloed, fragmented across systems, incompatible formats, and inaccessible at the moments it matters most.
AI tackles this by standardizing data formats, identifying relationships between disparate data points, and enabling real-time sharing across care settings. As Topflight Apps notes, healthcare organizations are reporting significant improvements in cross-system data accessibility after implementing AI-enhanced EHR solutions, without replacing existing infrastructure. AI augments rather than disrupts, fitting into current systems while dramatically expanding what those systems can do.
The Real Challenges of AI-EHR Integration
Data Privacy and Security in a High-Stakes Environment
Healthcare data is among the most sensitive information in existence. Integrating AI, which requires large datasets to train and operate effectively, into EHR systems creates genuine privacy risks that can't be hand-waved away with optimism about technology.
The stakes are high. HIPAA violations carry penalties up to $1.9 million per category per year, and a single breach can erode patient trust in ways that are difficult to rebuild. Key security requirements for AI-EHR integration include:
End-to-end encryption: Data must be protected both at rest and in transit. Any AI system processing patient data needs to meet or exceed the encryption standards required by HIPAA and, where applicable, GDPR
Strict access controls: Two-factor authentication, role-based access, and detailed access logs ensure only authorized personnel interact with sensitive data, and create accountability when something goes wrong
Data anonymization for model training: AI models can be trained on de-identified data, preserving the richness of the dataset while protecting individual privacy
Audit trails: Every AI interaction with patient data should be logged, reviewable, and attributable
The ONC's HTI-1 rule added algorithm transparency requirements for certified health IT in the U.S., and HHS published a sector-wide AI strategic plan in 2025. Regulatory clarity is improving, but organizations implementing AI must remain proactive rather than reactive about compliance.
High Implementation Costs and ROI Timelines
The upfront costs of AI-EHR integration are real. They include AI software licensing, infrastructure upgrades to support processing demands, staff training, and the ongoing work of maintaining and validating AI systems over time.
For smaller practices operating on tight margins, these costs can be prohibitive. The challenge is that ROI often takes months to materialize, and quantifying it requires measuring diffuse benefits like reduced burnout and fewer errors alongside more concrete metrics like billing speed and patient throughput.
The good news is that the economics are improving:
Embedded vendor AI: As Epic, Oracle Health, and athenahealth build AI natively into their platforms, many AI features will come at no additional licensing cost during EHR upgrades
Phased implementation: Scalable AI solutions allow organizations to start with high-ROI applications (like documentation or coding) and expand incrementally
Focus on measurable ROI drivers: Ambient scribes, for example, have clear financial justifications: more patient visits per day, faster billing cycles, and reduced physician turnover costs
Technical Complexity and Integration Friction
Not all EHR systems are built to integrate seamlessly with AI tools. Legacy infrastructure, common in community hospitals and smaller practices, often lacks the data architecture, processing capacity, or API connectivity that modern AI applications require.
Integration projects can disrupt clinical workflows during implementation. Staff resistance, especially from clinicians who remember poorly-designed EHR rollouts of the past, is also a real barrier. The AMA has been explicit that AI tools must be designed with clinician input, not imposed on them, a lesson the industry largely failed to learn with first-generation EHRs.
Key technical considerations include:
HL7 FHIR compliance: Modern interoperability standards are essential for AI to access and share EHR data effectively
API availability: AI tools need clean, well-documented APIs to connect with EHR platforms
Data quality: AI is only as good as the data it's trained on. EHRs with inconsistent documentation practices, missing fields, or legacy data entry errors create noisy training sets that degrade AI performance
AI Bias and Algorithmic Fairness
A challenge that has received increasing attention heading into 2026 is AI bias in clinical settings. AI models trained on historical healthcare data can inherit and amplify existing disparities, underperforming for underrepresented patient populations, misclassifying risk in minority groups, or making assumptions based on socioeconomic proxies embedded in the data.
Canadian health experts' "2025 Watch List" explicitly identified bias, fairness, and model reliability as urgent priorities. Healthcare organizations must demand bias audits from AI vendors, test models across diverse patient populations, and establish ongoing monitoring rather than treating fairness as a one-time check.
How EHR Vendors Are Responding: The Platform Shift
One of the most significant developments over the past year has been the move by major EHR platforms to build AI directly into their products. This is changing the calculus for every healthcare organization.
Epic Systems, which holds approximately 40% of the U.S. hospital EHR market, announced a major AI overhaul in mid-2025, featuring ambient scribes powered by Microsoft, a "doctor co-pilot" for order recommendations, a scheduling agent, and a patient-facing chatbot. Oracle Health (formerly Cerner) and athenahealth are making similar moves. In October 2025, athenahealth launched its own AI-powered features targeting clinical and administrative workflows.
What this means in practice:
AI is becoming table stakes: Hospitals that update their EHR will increasingly receive AI capabilities as part of the standard package
Third-party tools face pressure: Companies offering standalone AI tools, ambient scribes, coding tools, prior auth automation, must prove interoperability and integration quality as EHRs build competing native features
Lock-in risks are real: When AI functions are unique to one EHR, it creates dependency. Healthcare organizations should evaluate vendor AI carefully, with attention to data portability and performance transparency
The pace is accelerating: Ambient scribing alone generated $600 million in revenue in 2025, 2.4x year-over-year
The Role of AI Medical Scribes in EHR Integration
How Ambient AI Scribes Work
AI medical scribes represent the most mature and widely adopted application of AI in EHR integration today. They work by passively recording clinical conversations during patient visits, then using natural language processing (NLP) and large language models to generate structured clinical notes, HPI, ROS, physical exam findings, assessment, and plan, that are reviewed and approved by the clinician before being added to the EHR.
The workflow shift is significant. Instead of building documentation from memory after a visit (or during it, at the expense of eye contact and patient connection), clinicians validate AI-generated content and make targeted edits. Research published in JAMA found physicians saved an average of 3.2 hours per day on documentation using AI scribes. Studies also show that over 90% of patients prefer visits where their physician used an AI scribe, because the clinician is more present, engaged, and making eye contact rather than typing.
Key technologies powering ambient scribes:
Natural Language Processing (NLP): Understands and processes spoken medical language, including terminology, accents, and specialty-specific vocabulary
Large Language Models (LLMs): Generate structured, coherent clinical notes from conversational audio
Machine Learning: Models improve over time, learning from physician corrections and edits to increase accuracy with each use
EHR Integration APIs: Direct connections to EHR platforms ensure notes populate the right fields automatically without additional data entry
Reducing Clinician Burnout: The Evidence
The burnout case for AI scribes has moved from anecdotal to clinically validated. The Yale School of Medicine study published in JAMA Network Open in October 2025 is the largest multicenter evaluation to date, spanning 263 physicians across six health systems. The 74% reduction in burnout odds after 30 days of use is a remarkable finding for a technology intervention.
Mass General Brigham reported a 40% decline in reported burnout among physicians using AI transcription. UChicago Medicine found that ambient AI users experienced lower burnout and lighter cognitive load, with physicians reporting they were more focused throughout the day and "less mentally exhausted."
"Physicians notice the impact of having their cognitive load lightened. We're more focused throughout the day and less mentally exhausted, leaving more energy and compassion to dedicate to improving patients' quality of life." - UChicago Medicine researcher
A note of intellectual honesty: a 2025 review in Learning Health Systems cautioned that it may be premature to assert AI tools will universally reduce burnout, and that a controlled study at Atrium Health found no significant increase in physician throughput. The evidence is strong but not unanimous, and organizations should approach implementation with rigorous evaluation rather than assuming benefits will automatically materialize.
Enhancing EHR Documentation Quality
Beyond time savings, AI scribes improve documentation quality in ways that matter for patient care. Because they capture conversations in real time, rather than relying on clinician recall after the fact, AI-generated notes tend to be more complete, with fewer omissions and less variability across providers.
Consistent, comprehensive documentation supports better continuity of care, more accurate coding, and cleaner data for downstream AI analytics. In short, the more consistently good the input data is, the better every other AI application in the EHR performs.
Overcoming the Barriers: A Practical Framework
Start With High-ROI, Low-Disruption Use Cases
The organizations that succeed with AI-EHR integration typically don't try to transform everything at once. They identify the single most painful, highest-frequency workflow problem, usually documentation, and solve that first. Once clinical staff see real benefits, adoption of additional AI features becomes significantly easier.
Recommended entry points by impact:
Use Case | Typical ROI Driver | Integration Complexity |
|---|---|---|
Ambient AI scribes | Physician retention, billing speed | Low–Medium |
AI-assisted medical coding | Reduced denials, faster revenue cycle | Medium |
Predictive readmission alerts | Reduced penalties, better outcomes | Medium–High |
Prior authorization automation | Staff time savings, faster approvals | Medium–High |
Appointment scheduling AI | Staff efficiency, no-show reduction | Low |
Invest in Change Management, Not Just Technology
The AMA's lesson from first-generation EHR adoption is directly applicable to AI: technology imposed without clinical input creates resistance, workarounds, and adoption failure. Successful AI-EHR integration requires:
Physician champions: Identify early adopters who can demonstrate and advocate for AI tools to peers
Specialty customization: Generic AI models perform differently across specialties. Configuring tools for cardiology versus psychiatry versus primary care is essential for adoption and accuracy
Feedback loops: Regular mechanisms for clinical staff to flag errors, suggest improvements, and share experiences with AI tools
Transparent expectations: Be honest that AI tools require a learning curve and that initial performance may not reflect long-term capability
Build a Data Governance Framework First
Before implementing AI, organizations need clarity on how patient data will be handled: who can access it, how it's stored, how it's used in training, and how long it's retained. This isn't just a compliance exercise, it's the foundation that determines whether AI tools can legally and ethically operate in the first place.
A robust data governance framework includes:
Data classification: Identifying which data elements are protected health information (PHI) and how they flow through AI systems
Vendor agreements: BAAs (Business Associate Agreements) with all AI vendors who process PHI
Audit capabilities: The ability to review exactly what data any AI system has accessed and when
Bias monitoring: Ongoing evaluation of AI performance across patient demographic groups
What to Expect Through 2026 and Beyond: Where AI-EHR Integration Is Heading
Several trends are clearly accelerating heading into 2026:
Ambient-first documentation becomes the default. Industry analysts expect ambient documentation to be built into default EHR configurations at major vendors within the next 12–24 months. Organizations still using manual documentation will be in the minority.
AI agents go beyond documentation. The next wave of AI in EHR systems moves from documentation to action: AI agents that manage inbox messages, handle refill requests, coordinate referrals, and even interface with payer AI systems for prior authorization, all from within the EHR workflow.
Payer-provider AI integration. Menlo Ventures describes the emerging possibility of provider AI agents and payer AI agents communicating directly, automating prior authorization, utilization management, and claims adjudication in ways that could dramatically reduce administrative costs and care delays.
LLM-powered clinical decision support. Large language models like those powering Sully's AI platform are being adapted for real-time clinical decision support, summarizing patient records, flagging drug interactions, surfacing relevant clinical guidelines, and generating patient communication in plain language.
Equity and fairness requirements. Regulatory and payer pressure is building around algorithmic fairness in clinical AI. Expect more formal requirements around bias testing and demographic performance disclosure as part of AI procurement.
Frequently Asked Questions
What is AI integration with EHR systems?
AI integration with EHR systems refers to embedding artificial intelligence tools, such as ambient scribes, predictive analytics engines, and automated coding systems, directly into electronic health record workflows. Rather than replacing the EHR, AI augments it by automating documentation, identifying clinical patterns, and streamlining administrative tasks. By late 2025, 71% of U.S. hospitals were using at least one EHR-integrated AI tool.
How does AI improve efficiency in EHR systems?
AI improves EHR efficiency primarily by automating time-consuming tasks. Ambient scribes reduce documentation time by 15–50%, freeing clinicians for more patient-facing work. AI coding tools analyze clinical notes and suggest accurate billing codes, reducing claim denials. Predictive models surface high-risk patients proactively, allowing care teams to intervene earlier and avoid costly complications. Together, these tools address the two biggest efficiency drains in healthcare: documentation burden and administrative overhead.
What are the biggest challenges of integrating AI with EHR systems?
The most significant challenges are data privacy and security (ensuring AI systems handling PHI comply with HIPAA and other regulations), high upfront implementation costs, technical integration friction with legacy systems, and the risk of AI bias if models are trained on unrepresentative data. Change management, getting clinical staff to trust and use new AI tools, is also consistently cited as a barrier in healthcare organizations.
What is an AI medical scribe and how does it work with the EHR?
An AI medical scribe is an ambient tool that listens to patient-provider conversations during clinical visits and automatically generates structured clinical notes. Using NLP and large language models, it drafts the HPI, physical exam findings, assessment, and plan, which the clinician reviews and approves before the note is committed to the EHR. Studies show physicians save an average of 3.2 hours per day on documentation using these tools, and a Yale study found burnout dropped 74% in odds after just 30 days of use.
Is AI integration with EHR systems HIPAA compliant?
It can be, but compliance is not automatic, it requires deliberate design and vendor accountability. AI systems that process patient data must operate under Business Associate Agreements, use appropriate encryption, enforce strict access controls, and maintain audit logs. The ONC's HTI-1 rule now adds algorithm transparency requirements for certified health IT, and HHS published a sector-wide AI strategic plan in 2025. Organizations should perform thorough due diligence on any AI vendor's compliance posture before implementation.
How much does it cost to implement AI in an EHR system?
Costs vary significantly by scope and vendor. Standalone ambient scribe tools often charge per-physician monthly subscription fees (typically $200–$500/month per provider). Enterprise-wide implementations integrating predictive analytics, coding AI, and workflow automation can run into the hundreds of thousands to millions of dollars. However, the economics are improving: as Epic, Oracle Health, and athenahealth embed AI natively into their platforms, many features will come as part of standard EHR contracts at no additional licensing cost.
Which EHR systems currently support AI integration?
All major EHR platforms are building or have built AI capabilities as of early 2026. Epic announced a major AI overhaul featuring ambient scribes (powered by Microsoft), clinical copilots, and scheduling agents. Oracle Health and athenahealth have also launched AI-powered documentation and workflow tools. Alongside these native capabilities, third-party AI platforms including Sully's AI agents integrate with most major EHR systems via HL7 FHIR APIs and direct partnerships.
Sources
[1] Menlo Ventures: 2025: The State of AI in Healthcare. Comprehensive market analysis of AI adoption across healthcare verticals. https://menlovc.com/perspective/2025-the-state-of-ai-in-healthcare/
[2] Toward Healthcare: U.S. AI in Healthcare Market Sizing and Forecast to 2034. https://www.towardshealthcare.com/insights/us-ai-in-healthcare-market-sizing
[3] IntuitionLabs: AI in Hospitals: 2025 Adoption Trends & Statistics. https://intuitionlabs.ai/articles/ai-adoption-us-hospitals-2025
[4] IntuitionLabs: AI in Hospital Operations: 2025 Trends, Efficiency & Data. https://intuitionlabs.ai/articles/ai-hospital-operations-2025-trends
[5] TATEEDA Global: 2026 AI Trends in US Healthcare. https://tateeda.com/blog/ai-trends-in-us-healthcare
[6] Yale School of Medicine: AI Scribes Reduce Physician Burnout and Return Focus to the Patient (JAMA Network Open, October 2025). https://medicine.yale.edu/news-article/ai-scribes-reduce-physician-burnout-return-focus-to-the-patient/
[7] University of Chicago Medicine: Studies suggest ambient AI saves time, reduces burnout and fosters patient connection (JAMA Network Open, October 2025). https://www.uchicagomedicine.org/forefront/research-and-discoveries-articles/ambient-ai-saves-time-reduces-burnout-fosters-patient-connection
[8] American Medical Association: Physician burnout solutions: Using AI to improve EHR workflows. https://www.ama-assn.org/practice-management/digital-health/physician-burnout-solutions-using-ai-improve-electronic-health-0
[9] Anzolo Medical: AI-Powered EHR Documentation: How Healthcare Organizations Are Achieving 40% Time Savings in 2025. https://business.anzolomed.com/ai-powered-ehr-documentation-how-healthcare-organizations-are-achieving-40-time-savings-in-2025/
[10] ForseeMed: Artificial Intelligence in Healthcare & Medical Field. https://www.foreseemed.com/artificial-intelligence-in-healthcare
[11] Grand View Research: AI in Healthcare Market Size & Share Report, 2033. https://www.grandviewresearch.com/industry-analysis/artificial-intelligence-ai-healthcare-market
[12] Topflight Apps: AI in EHR: Benefits, Costs, Use Cases for Smarter Electronic Health Records. https://topflightapps.com/ideas/ai-in-ehr/
[13] SPRY PT: AI Medical Scribes: How They Work, Benefits, Top Solutions, and Implementation Guide. https://www.sprypt.com/blog/ai-medical-scribe-the-ultimate-guide-for-healthcare-providers
[14] TempDev: Improving Patient Care & Reducing Physician Burnout with AI. https://www.tempdev.com/blog/2025/04/04/ai-healthcare-reducing-physician-burnout-enhancing-patient-care/
[15] Frontiers in Public Health: Impact of artificial intelligence on EHR-related burnout among healthcare professionals: systematic review (2025). https://www.frontiersin.org/journals/public-health/articles/10.3389/fpubh.2025.1628831/full
[16] PMC / Learning Health Systems: Artificial intelligence and physician burnout: A productivity paradox (2025). https://pmc.ncbi.nlm.nih.gov/articles/PMC12569468/
[17] SNS Insider / GlobeNewswire: Artificial Intelligence in Healthcare Market Size to Reach USD 1222.12 Billion by 2035 (March 2026). https://www.globenewswire.com/news-release/2026/03/04/3249111/0/en/Artificial-Intelligence-in-Healthcare-Market-Size-to-Reach-USD-1222-12-Billion-by-2035
TABLE OF CONTENTS
Hire your
Medical AI Team
Take a look at our Medical AI Team
AI Receptionist
Manages patient scheduling, communications, and front-desk operations across all channels.
AI Scribe
Documents clinical encounters and maintains accurate EHR/EMR records in real-time.
AI Medical Coder
Assigns and validates medical codes to ensure accurate billing and regulatory compliance.
AI Nurse
Assesses patient urgency and coordinates appropriate care pathways based on clinical needs.